
A Data-Driven Approach to Intertrochanteric Fracture Rehabilitation for the Modern Clinic
Treatment GuidelinesExplore evidence-based rehab protocols for elderly intertrochanteric fractures, improving recovery, outcomes, and reducing complications.
Intertrochanteric fractures in elderly patients require comprehensive rehabilitation beyond surgical repair, typically led by physical therapy (PT) and occupational therapy (OT) working together to restore mobility and independence.
This guide provides evidence-based protocols for each recovery phase, emphasizing early mobilization, objective progress tracking, and holistic patient care.
We explore how modern rehabilitation technology helps clinicians deliver measurable outcomes while addressing the physical, psychological, and functional needs of elderly hip fracture patients.
From Surgical Success to Functional Independence
Every year, over 280,000 older adults are hospitalized for hip fractures, with intertrochanteric fractures accounting for nearly half of these cases. While surgical stabilization gets the headlines, we know the real work begins when patients arrive at your clinic. This is where PT and OT become central to intertrochanteric fracture treatment in elderly patients, translating surgical success into meaningful functional recovery.
The shift from surgical success to functional independence defines excellence in rehabilitation. Your role extends far beyond following standard protocols; you’re orchestrating a complex recovery that determines whether your patient returns to independent living or faces long-term disability. This guide moves past basic medical descriptions to provide you with a strategic framework for optimizing recovery, demonstrating value through objective data, and streamlining your care pathway.
What OT & PT Rehab Professionals Must Know About the Surgery
For physical therapists and occupational therapists, understanding surgical fixation choices is essential for safe progression of mobility, ADLs, and weight-bearing activities.
Decoding the Diagnosis and Fracture Type
Understanding fracture stability directly impacts your rehabilitation planning. Stable fractures allow for more aggressive early mobilization, while unstable patterns require careful progression. When you review that operative report, you’re looking for key details: Was internal fixation achieved with a sliding hip screw or intramedullary nail? Did the surgeon opt for arthroplasty due to poor bone quality?
Surgical Interventions and Their Rehab Implications
Internal Fixation Considerations: The hardware choice significantly impacts your weight-bearing progression. A sliding hip screw typically allows controlled weight-bearing earlier than you might expect, while intramedullary nailing provides excellent stability for subtrochanteric extension. Your therapy approach must account for potential hardware failure risks, particularly in osteoporotic bone.
Arthroplasty Implications: When surgeons choose hemiarthroplasty or total hip replacement for severely comminuted fractures, your protocols shift. Dislocation precautions become paramount, and you’ll need to educate patients on hip precautions that may last a lifetime.
The key takeaway? Translate that operative report into a rehabilitation plan that respects surgical constraints while pushing toward functional goals.
The Rehab Team’s Role in the Acute Phase
The Critical Handoff
Collaboration between PTs, OTs, surgeons, and nursing teams sets the recovery trajectory for elderly patients following intertrochanteric fracture surgery. Research from The American Academy of Orthopaedic Surgeon’s Clinical Practice Guidelines shows that interdisciplinary collaboration reduces post-surgical complications and improves patients’ outcomes.
Early mobilization within the first 24–48 hours after hip surgery is highly recommended. Studies show that early mobilization contributes to several critical benefits, including:
- Shorter length of stay
- Fewer post-op complications
- Less pain
- Better walking stability
- Higher quality of life
- Lower hospitalization costs
- Lower chance of readmission
Initial Bedside Protocol
Starting rehabilitation while patients are still in the hospital requires careful assessment and progression. Begin with:
- Pain assessment and positioning strategies
- Safe transfer training with appropriate assistive devices
- Initial weight-bearing assessment based on surgical parameters
- Essential exercises: ankle pumps, quadriceps sets, and gluteal contractions
Building the Evidence-Based Rehab Protocol: A Phased Approach to Recovery
Phase I: Protection and Activation (Weeks 0-4)
Your initial goals focus on controlling pain and edema while maintaining joint mobility and muscle activation. During this phase, PT focuses on early mobility, gait training, and strength activation, while OT addresses bed mobility, toileting, dressing strategies, and adaptive techniques to promote early independence. With this combination, you’re establishing the foundation for recovery.
Specific Interventions:
- Gait training with appropriate therapeutic devices
- Isometric strengthening focusing on hip and knee musculature
- Active-assisted range of motion exercises within surgical precautions
Objective Measurement: Track pain levels using validated scales, measure gait distance, and document assistance levels. The PrimusRS allows you to objectively measure isometric
strength even in early phases, providing baseline data that guides your progression decisions.

Phase II: Progressive Strengthening and Weight-Bearing (Weeks 4-8)
As surgical healing progresses, your focus shifts to rebuilding strength and normalizing movement patterns. In this phase, physical therapy intensifies lower-extremity strengthening and gait normalization, while occupational therapy progresses instrumental ADLs such as bathing, meal preparation, and home task simulation.
Targeted Exercises:
- Closed-chain exercises like mini-squats and weight shifts
- Progressive single-leg stance activities
- Gradual weaning from assistive devices
Progress Tracking: Implement standardized tests like the Timed Up and Go (TUG) and 5x Sit-to-Stand. The Eccentron provides controlled eccentric strengthening for the lower extremities, particularly valuable for elderly patients who benefit from the lower cardiovascular demand of eccentric exercise.

Phase III: Functional Restoration and Fall Prevention (Weeks 8+)
This phase emphasizes returning patients to community-level function while addressing fall risk, the primary concern for this population. This stage requires close coordination between PT and OT, with PT emphasizing balance, endurance, and community ambulation, and OT focusing on fall prevention strategies, home safety, and functional confidence in daily routines.
Advanced Interventions:
- Uneven surface navigation
- Stair negotiation training
- Dual-task activities combining cognitive and physical challenges
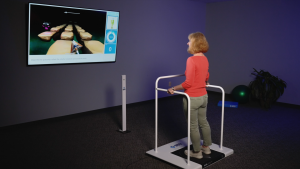
Functional Assessment: The Berg Balance Scale and functional reach tests provide objective data on fall risk. The Alfa balance platform helps you deliver targeted balance training via interactive therapeutic gaming, allowing patients to self-correct and visualize their progress while you collect objective stability data.
The Power of Objective Data: Proving Value and Personalizing Care
For the Practitioner: Moving from “Feels Better” to “Is Better”
You know patients often underestimate or overstate their progress. Objective testing eliminates guesswork. When you document a 30% improvement in TUG time or demonstrate increased hip abductor strength through dynamometry, you’re providing concrete evidence of progress that motivates patients and justifies continued care.
Systems like PrimusRS help you perform comprehensive functional evaluations with automated reporting, transforming subjective observations into objective, defensible documentation.

For the Clinic Owner: Demonstrating Outcomes, Driving Revenue
Your ability to show measurable outcomes differentiates your clinic. Aggregate patient data demonstrating consistent functional improvements becomes powerful marketing material for orthopedic surgeon referrals. Clean, objective progress reports support reimbursement claims and reduce denials.
For Hospital Administrators: Standardization and Compliance
Data-driven protocols allow standardization across multiple facilities while maintaining individualized care. Clear metrics on departmental performance simplify compliance reporting and quality improvement initiatives.
Treating the Patient, Not Just the Fracture
Th PT’s Critical Role
Physical therapy plays a foundational role in intertrochanteric fracture treatment in elderly patients, targeting strength restoration, gait mechanics, balance retraining, and fall-risk reduction. PT interventions directly influence mobility outcomes, discharge disposition, and long-term independence.
The Eccentron helps physical therapists restore the strength foundation needed for safe ambulation and independence, while respecting the physiological limitations of older adults.
The OT’s Critical Role
Occupational therapy addresses the practical aspects of recovery that determine independence, such as:
- ADL retraining with adaptive equipment
- Home safety assessments and modifications
- Cognitive strategies for complex task management
The Simulator II helps occupational therapists replicate daily tasks and job-specific activities, providing objective measurement of functional abilities.

Addressing the Psychological Barrier
Fear of falling affects up to 73% of hip fracture patients, often limiting recovery more than physical constraints. Your approach should include:
- Confidence-building through graded exposure
- Education about realistic fall risk
- Screening for depression and anxiety
Building confidence requires showing patients their objective progress. When elderly patients see their balance scores improving on visual displays, fear diminishes and engagement increases.
Fueling the Recovery
Nutrition plays a crucial yet often overlooked role in fracture healing. Ensure your patients understand:
- Protein requirements increase to 1.2-1.5g/kg body weight during healing
- Calcium and Vitamin D supplementation supports bone remodeling
- Adequate caloric intake prevents muscle wasting
Partner with dietitians to provide comprehensive nutritional guidance that supports your rehabilitation efforts.
Patient-Centered Goal Setting
Success means different things to different patients. For one, it’s walking to the mailbox independently. For another, it’s returning to golf. Collaborate with patients and families to establish meaningful, measurable goals that drive engagement.
The Multi-Cervical Unit might seem unrelated to hip fractures, but remember that elderly patients often present with multiple musculoskeletal issues. Comprehensive assessment ensures you’re addressing all factors affecting function.
Special Considerations for the Elderly Population
Comorbidity Management
Your elderly hip fracture patients rarely present with isolated injuries. Diabetes affects wound healing, cardiovascular disease limits exercise tolerance, and cognitive impairment impacts learning ability. Successful rehabilitation requires adapting protocols to accommodate these challenges while maintaining therapeutic intensity.
Medication Implications
Polypharmacy in elderly patients creates unique challenges. Beta-blockers may limit heart rate response to exercise, while anticoagulants increase fall risk concerns. Regular communication with medical providers ensures your therapy remains aggressive yet appropriate.
Technology Integration for Enhanced Outcomes
Modern rehabilitation technology transforms how we deliver care to elderly hip fracture patients. The Alfa balance system demonstrates how gamification principles engage elderly patients who might otherwise resist traditional exercise programs.

Objective measurement systems provide immediate feedback that helps elderly patients understand their progress. Real-time visual displays make abstract concepts like weight distribution or postural control concrete and understandable.
Conclusion: Elevating the Standard of Hip Fracture Rehabilitation
Successful intertrochanteric fracture treatment in elderly patients depends on coordinated physical therapy and occupational therapy, supported by objective data and patient-centered goal setting. Your modern practice has access to tools that facilitate recovery while proving value objectively.
The elderly patient recovering from an intertrochanteric fracture represents one of rehabilitation’s greatest challenges and opportunities. By combining evidence-based protocols with objective measurement technology, addressing psychological barriers alongside physical limitations, and maintaining focus on functional independence, you’re not just helping patients heal; you’re restoring their quality of life.
Ready to implement standardized, data-driven protocols for your hip fracture patients? Discover how BTE’s comprehensive testing and rehabilitation systems provide the objective data and progress tracking tools to elevate your outcomes and grow your practice. Your elderly patients deserve rehabilitation that’s as sophisticated as their surgery, and you have the knowledge and tools to deliver it.
Frequently Asked Questions about Intertrochanteric Fracture Treatment in Elderly Patients
1. When can we start weight-bearing activities after intertrochanteric fracture surgery?
Weight-bearing status depends on the surgical fixation method and surgeon’s protocol. Most patients with stable internal fixation (intramedullary nails or dynamic hip screws) can begin partial weight-bearing within 24-48 hours post-surgery. Always verify the specific weight-bearing restrictions with the orthopedic surgeon before initiating therapy. Progressive weight-bearing typically advances from toe-touch to partial (25-50% body weight) to full weight-bearing over 6-12 weeks, based on fracture healing and patient tolerance.
2. What are the key safety precautions during early mobilization?
Monitor for signs of implant failure, increased pain, or loss of reduction. Ensure proper use of assistive devices and maintain prescribed weight-bearing limits. Watch for symptoms of deep vein thrombosis (leg swelling, warmth, redness). Use gait belts during transfers and ambulation training. Assess for orthostatic hypotension before standing activities. Avoid hip flexion beyond 90 degrees and extreme rotation movements that could stress the surgical site.
3. How do we address the high fall risk in these patients?
Implement comprehensive fall prevention strategies including balance training, lower extremity strengthening, and gait training with appropriate assistive devices. Conduct home safety evaluations and recommend environmental modifications like grab bars, adequate lighting, and removal of trip hazards. Address vision impairments and review medications that may affect balance. Educate patients and caregivers about fall prevention techniques and the importance of using prescribed assistive devices consistently.
4. What functional outcomes should we expect and track?
Key metrics include return to pre-fracture mobility level, independence in ADLs, walking distance and speed, and ability to navigate stairs. Use standardized assessments like the Functional Independence Measure (FIM), Timed Up and Go test, and 6-minute walk test. Expect gradual improvement over 3-6 months, with most functional gains occurring in the first 12 weeks. Document pain levels, range of motion, strength measurements, and balance scores to track progress objectively.
5. How long does the rehabilitation process typically take?
Acute rehabilitation typically lasts 1-3 weeks in inpatient settings, followed by outpatient therapy for 6-12 weeks. Total recovery time varies from 3-6 months depending on patient factors like age, pre-fracture function, comorbidities, and bone healing. Early mobilization within 24-48 hours is crucial for optimal outcomes. Patients may continue with maintenance exercises and fall prevention programs long-term to preserve gains and prevent future fractures.
6. What adaptive equipment and home modifications are most beneficial?
Essential equipment includes raised toilet seats, shower chairs or benches, grab bars in bathrooms, and appropriate assistive devices for ambulation (walker, cane, or crutches). Recommend removing throw rugs, improving lighting, installing handrails on stairs, and ensuring clear pathways. Consider bed rails for safe transfers, long-handled reaching tools, and sock aids for patients with limited hip flexion. Collaborate with occupational therapy for comprehensive home safety assessments and equipment recommendations.






