Strength Testing: A Guide to Manual Muscle Testing and Dynamometry
Treatment GuidelinesUnderstand manual muscle testing and dynamometry protocols. Learn how to assess muscle strength with precise grading and objective measurement tools.
In the rehab field, practitioners have a variety of tools with which they can quantify strength. One of these tools, known as MMT or manual muscle testing, is a low-tech method which relies on a somewhat subjective interpretation by the clinician. Another method is dynamometry, which uses a range of equipment to more objectively assess a patient’s strength.
Both methods have their potential benefits, and their potential downsides. In this post, we’ll take a look at MMT and dynamometry to provide clinicians with an informational guide on this important subject.
The Evolution of MMT: From Ancient Practices to Modern Rehab
MMT was first used and described in the early 20th century to gauge weakness in polio patients. From there, the method was refined to enable different practitioners to get as accurate an assessment of a patient’s strength as possible. The technique was further expanded for use on other patients, such as those who had suffered neuromuscular injuries or were experiencing weakness for any reason.
What is Manual Muscle Testing (MMT)?
Manual Muscle Testing (MMT) is the most widely used method for documenting muscle strength deficits in rehabilitation. It is a standardized clinical procedure where a therapist applies resistance to a patient’s limb to grade their strength on a specific scale.
Unlike strength training, which builds muscle, MMT is a diagnostic tool used to:
- Identify Weakness: Pinpoint specific muscles or muscle groups that are underperforming due to injury, atrophy, or neurological impairment.
- Establish a Baseline: Create a starting point for therapy to measure progress against.
- Localize Lesions: In neurology, patterns of weakness found during MMT can help localize nerve damage (e.g., differentiating a peripheral nerve injury from a spinal root injury).
While simple in concept, MMT requires a high degree of skill. The clinician must understand line-of-pull, proper stabilization, and anatomy to isolate the target muscle and avoid “compensation” (where strong muscles take over for weak ones). Because it relies on the therapist’s perception of effort, it is often described as a “subjective” measure, though standardized grading scales (like the Oxford Scale) attempt to make it as objective as possible.
How to Perform MMT Like a Pro: Techniques and Best Practices
Because MMT relies on the clinician’s own muscular strength, body mechanics are paramount. The therapist should ensure that they position themselves in such a way so as to minimize stress on their own joints, while also being mindful of the patient’s comfort and positioning.
MMT is a useful tool for degenerative diseases which can progress quickly (both in terms of improvement and worsening). By frequently monitoring a patient’s strength from day to day, practitioners can gather meaningful data on the progression of conditions such as ALS, muscular dystrophy, or spinal cord injuries to name a few.
Guide to Performing MMT
There are a few key principles to keep in mind when it comes to MMT. Namely, the therapist must ensure that the patient:
- Has adequate range of motion in the joint of interest.
- Is able to get into a position where they can activate the muscle, moving the limb against the force of gravity.
For instance, when testing the strength of the biceps brachii. The following steps should be followed:
- Have the patient seated comfortably, while the therapist stands.
- Ensure that the patient has adequate passive and active range of motion of the elbow joint.
- Assuming that range of motion is normal, have the patient fully flex their elbow, with the forearm supinated.
- The patient is instructed to maintain this position, while the therapist attempts to pull the elbow into extension and rotate the forearm into pronation. The therapist’s other hand should stabilize the patient’s shoulder.
- The patient’s muscle strength is then graded, according to one of the systems described in the next section.
Grading Systems
There are a few recognized grading systems for manual muscle testing, such as the Oxford Scale and the Medical Research Council Scale.
Oxford Scale
The Oxford Scale uses a 0-5 grading system.
- 0/5 indicates no muscle activity.
- 1/5 indicates muscle activity without any joint motion.
- 2/5 indicates joint movement in the gravity eliminated position.
- 3/5 indicates the ability of the joint to move against gravity, without extra resistance.
- 4/5 indicates the ability of the joint to move against light resistance.
- 5/5 indicates the ability of the muscle to resist heavy push back.
Medical Research Council Scale
The Medical Research Council Scale uses a similar 0-5 grading system to the Oxford Scale. However, there are slight differences in the descriptions of a patient’s strength, especially at the higher levels of strength. For clinical purposes, these scales ultimately end up being about the same. They can differ slightly when it comes to more in depth research studies.
Make vs. Break MMT: Key Differences and When to Use Each
Under the umbrella of MMT, there are “make” tests and “break” tests. Most therapists will use these tests with fluidity, selecting one or the other depending on the specific nature of the patient’s condition.
The Make Test
The make test involves holding constant resistance against the patient’s fully contracted muscle. This allows the therapist to determine the patient’s isometric strength.
The Break Test
The break test involves the therapist applying more and more resistance against the patient’s fully contracted muscle in an attempt to push them out of the position. This tests isometric strength in addition to eccentric strength of the involved muscle.
Why Objective Strength Testing Matters
Having accuracy in data collection is important in all fields. For this reason, it is best to not rely solely on subjective measures, such as manual muscle testing, when assessing a patient’s strength. Better data during examination and evaluation often leads to better patient outcomes.
The Power of Dynamometry: Precision Testing for Optimal Results
Dynamometers provide a numerical value for strength which is generally considered both reliable and valid. Besides the convenience of MMT, dynamometry is much more preferable for strength testing in virtually every way.
As long as the equipment is well-maintained and the proper testing protocols are followed, the machine will give an accurate read out of the patient’s strength whenever they are tested. This is crucial for baseline measurements, discharge planning, and for generally assessing the patient’s response to treatment.
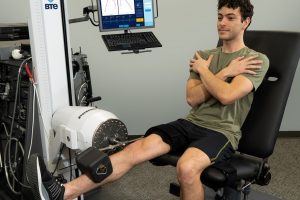
Fixed Dynamometers: Gold Standard for Reliable Strength Assessment
A fixed dynamometer is a complex piece of equipment, rarely seen outside of a research setting. These devices are very accurate for testing strength and are often considered a gold standard against which other methods can be measured. Fixed dynamometers such as the PrimusRS are attached to large, stable structures to ensure that they are not moved or affected during testing and use.
Portable Fixed Dynamometers: Take Accurate Testing Anywhere
When research needs to be conducted in a field setting, a portable fixed dynamometer fits the bill. These devices allow for accurate strength testing on the go, meeting athletes and patients in more applicable settings.
Billing and Reimbursement: The Financial Side of Strength Testing
Moving from subjective MMT to objective dynamometry doesn’t just improve clinical care; it can also support a more robust billing strategy. While MMT is typically bundled into a standard evaluation, objective testing opens the door for specific performance-based codes.
Understanding CPT 97750
The most relevant code for objective strength analysis is CPT 97750 (Physical Performance Test or Measurement).
- When to use it: This code is distinct from therapeutic exercise. It is used when you are performing a specific test that produces a written report and data analysis to guide the plan of care.
- Why it matters: 97750 generally has a higher reimbursement rate than standard exercise codes (like 97110), reflecting the clinical expertise and technology required to perform the test and analyze the findings.
Insurance auditors are increasingly scrutinizing claims for “lack of progress.” Subjective notes (e.g., “Patient strength is 4/5”) are often deemed insufficient to justify continued therapy.
A dynamometry report stating, “Patient demonstrates a 25% strength deficit in the involved shoulder compared to the uninjured side,” provides undeniable, quantitative proof of medical necessity. This level of documentation is critical for preventing claim denials and justifying extended plans of care.
Handheld Dynamometers: Pros, Cons, and When to Use Them
These portable devices are extremely convenient for clinicians and easy to use for patients. However, they may be less reliable when used for testing certain body areas, and repeatability can vary when compared to fixed assessment devices. These are great tools to use throughout a patient’s rehab program for many conditions, especially when a fixed dynamometer is unavailable.
The “Therapist Strength” Limitation
Handheld Dynamometers (HHD) are a major upgrade over MMT, but they have a distinct physical limitation: You.
In order to get an accurate reading, the therapist must be stronger than the muscle group being tested. If a therapist cannot hold the device completely still against the patient’s force (stabilization), the reading will be artificially low. This is particularly problematic when testing strong muscle groups like the quadriceps or plantar flexors in athletic populations.
Fixed Dynamometers eliminate this variable by removing the clinician from the force equation entirely, ensuring the measurement reflects the patient’s true maximum output, not the therapist’s maximum resistance.
Research Comparing Fixed, Portable, and Handheld Tools
The findings in the current available research on dynamometry generally confirms what one might logically assume:
- Fixed devices, when compared to handheld tools, tend to be more reliable and valid when determining a patient’s strength.
- Handheld tools are more widely available, and tend to be more user friendly for patients.
- Standardization may be lacking in some handheld devices, and ceiling effects may affect results.
Choosing the Right Strength Testing Method
Which strength testing method is right for your practice? This will depend on a variety of factors. If you need extremely accurate data, and your budget permits, you might lean toward a fixed or portable fixed dynamometer. If your practice requires more field work and you need less cumbersome tools (and are willing to sacrifice some potential accuracy in data collection), you may opt for a handheld device.
When investing in strength testing equipment, the “best” tool depends entirely on your specific clinical population and facility goals. Whether you are considering a simple handheld unit or a comprehensive fixed system, evaluate your purchase based on these three critical factors:
1. Stabilization and Repeatability
This is the most important factor for data accuracy.
- Handheld Considerations: If your clinic treats high-level athletes or strong industrial workers, a handheld dynamometer (HHD) may not be sufficient. If the patient is stronger than the therapist, the data will be invalid. Look for HHDs that come with belt-stabilization straps to mitigate this issue.
- Fixed System Considerations: For research centers and high-performance clinics, fixed systems offer the highest level of stabilization. By removing the therapist from the physical equation, you ensure that a measurement taken today is perfectly comparable to one taken next month, regardless of which staff member performs the test.
2. Workflow Efficiency and Software
Advanced technology is useless if it creates a bottleneck in your clinic schedule.
- Data Integration: Does the device export data easily to your EMR, or will you have to manually type numbers into a computer?
- Report Generation: Look for systems that generate automatic, patient-friendly reports. A graphical report that visualizes strength deficits is a powerful tool for patient education and compliance.
Peruse our testing products and choose the right physical or occupational therapy assessment tools for your practice.