
Therapy Equipment for Parkinson's: Enhancing Patient Mobility
Treatment GuidelinesGuide to Parkinson’s therapy equipment for PT Clinics: enhance mobility, manage symptoms, and integrate evidence-based rehab solutions.
Investing in Parkinson’s therapy equipment is a strategic decision for physical therapy clinic directors. While effective Parkinson’s rehabilitation can absolutely be delivered with minimal equipment, strategically chosen equipment can differentiate your clinic in a competitive referral landscape.
Here’s what matters: specialized equipment signals to neurologists and patients that you’re serious about Parkinson’s care. Quantifiable balance assessments, objective functional movement data, and technology-enhanced training create tangible differentiation that modest programs struggle to achieve. The right equipment doesn’t just improve outcomes, it positions your clinic as a specialized destination for Parkinson’s rehabilitation.
That said, you don’t need high-tech gadgets across the board. The most impactful approach combines foundational, versatile equipment that serves multiple patient populations with strategic investments in Parkinson’s-specific systems.
Understanding Equipment Needs Across Disease Stages
Parkinson’s disease presents progressively, meaning equipment needs evolve as symptoms advance. Early-stage patients (stages 1-2 on Hoehn and Yahr scale) benefit most from functional task-based training that emphasizes movement amplitude, balance, functional strengthening, and relaxation techniques. As the disease progresses to mid and late stages (stages 3-4), patients require more assistance with transfers, closer supervision during tasks, and more supportive mobility devices.
This progression directly impacts your equipment purchasing decisions. Start with versatile, foundational equipment that serves patients across multiple stages rather than investing heavily in stage-specific technology.
The Foundation: Balance Systems and Cueing Tools
Balance training equipment is a great investment option for Parkinson’s rehabilitation. Research consistently demonstrates that balance deficits are associated with a 68% fall rate among people with Parkinson’s disease,1 making balance intervention both clinically and financially justified.
Dynamic Balance Platforms
The Alfa balance platform provides objective balance assessments with built-in therapeutic gaming to address balance, postural control, and proprioception. These systems offer quantifiable progress tracking, essential for demonstrating medical necessity and justifying continued treatment to payers.
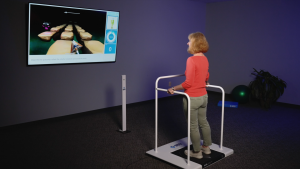
Balance platforms serve multiple patient populations beyond Parkinson’s, maximizing ROI through versatility. The same equipment supports vestibular rehabilitation, post-surgical orthopedic patients, and fall prevention programs.
Visual and Auditory Cueing Devices
Cueing represents one of the most evidence-supported interventions for Parkinson’s gait disturbances, particularly for addressing freezing episodes. Simple visual cues (laser lines, floor markers) and auditory cues (metronomes, rhythmic music) can be implemented with minimal investment—often under $200 for quality equipment.
The key is systematic implementation rather than expensive technology. Staff training on proper cueing strategies matters more than sophisticated devices.
LSVT BIG: Open Space Over Equipment
LSVT BIG therapy has demonstrated significant improvements in motor function, proprioceptive performance, and quality of life in people with Parkinson’s disease. The protocol focuses on amplitude-based training—teaching patients to move with exaggerated, large-scale movements to combat bradykinesia and hypokinesia.
Here’s the critical point for equipment planning: LSVT BIG requires minimal specialized equipment. The protocol succeeds through highly specific, one-on-one training emphasizing maximal amplitude movements, repetitive multidirectional patterns, and goal-directed activities of daily living.
What you actually need:
- Open floor space for full-body movement patterns
- Mirrors for visual feedback
- Simple props (cones, targets, reaching objects)
- Basic resistance bands
Boxing Equipment: Group Classes
Boxing-based programs like Rock Steady Boxing have gained substantial attention in Parkinson’s rehabilitation, supported by emerging research demonstrating improvements in balance, gait, motor function, and non-motor symptoms2 including depression and quality of life.
Equipment requirements remain modest:
- Heavy bags or standing bags
- Speed bags (optional but popular with patients)
- Boxing gloves
- Floor space for footwork drills
- Basic strength training equipment (resistance bands, light dumbbells)
The program is effective and offers strong community support without needing costly equipment.
Strength Training Equipment: Strategic Versatility
For Parkinson’s patients dealing with bradykinesia, rigidity, and reduced functional capacity, strength training equipment that emphasizes eccentric training offers unique benefits.
Eccentric-Focused Systems
The Eccentron is designed for eccentric training, which suits patients with low aerobic capacity or lower limb weakness. This method enables higher force with less cardiovascular demand, making it effective for those who are deconditioned or in advanced disease stages.

However, eccentric training represents one option among many. Standard resistance training equipment—cable systems, adjustable benches, free weights—serves Parkinson’s patients effectively when incorporated into evidence-based protocols focusing on eccentric versatility in rehabilitation.
Multi-Function Trainers
The PrimusRS offers multi-use functional training for both upper and lower extremities with the ability to practice ADLs in the clinic. This versatility makes it valuable for comprehensive Parkinson’s programs addressing strength, coordination, and functional task practice.

Upper Extremity and Fine Motor Equipment
Parkinson’s disease significantly impacts upper extremity function, creating difficulties with handwriting, buttoning clothes, and manipulation tasks. Addressing these deficits requires equipment supporting fine motor skill development and proprioceptive training.
Functional Upper Extremity Systems
The Simulator II provides functional rehabilitation targeting upper extremity strength, range of motion, and functional task practice. Patients can practice specific ADLs in the clinic to regain independence in daily activities.
The Capri addresses upper extremity proprioception and motor control through therapeutic gaming—particularly valuable for addressing the proprioceptive dysfunction common in Parkinson’s disease.

Marketing and Referral Development
Referral patterns favor clinics that can demonstrate specialized expertise through objective, quantifiable outcomes.
Positioning your clinic as a Parkinson’s specialist requires more than listing available services—it requires demonstrable measurement capacity. Physicians respond to data. When you can provide referring neurologists with quantified balance improvements, gait velocity changes, and objective functional measures, you build trust and credibility that goes a long way.
Demonstrate outcomes through:
- Quantifiable balance improvements (balance platform data)
- UPDRS motor score changes
- Functional mobility metrics (TUG, gait speed, endurance)
- Patient-reported quality of life measures
These outcomes attract referrals more effectively than equipment lists.
The Bottom Line
Effective Parkinson’s rehabilitation exists on a spectrum. At one end, skilled therapists deliver evidence-based protocols with minimal equipment investment and still reach meaningful functional improvements. At the other end, clinics leverage specialized equipment to enhance outcomes while simultaneously building a competitive advantage that attracts referrals and establishes market position.
The strategic question is whether you want to position your clinic as a general rehabilitation provider that sees Parkinson’s patients, or as a specialized Parkinson’s destination that neurologists actively seek out for their newly diagnosed patients.
Specialized equipment creates this differentiation. Balance platforms provide objective data and real time feedback. Gait analysis systems generate quantifiable metrics that demonstrate expertise. Technology-enhanced training signals investment in cutting-edge care. The best part is that this equipment can be used across multiple populations. These advantages translate directly into referral volume, patient retention, and premium positioning in your market.
Martin Gonzalez, DPT, Cert DN, is a board-certified physical therapist and health writer specializing in chronic pain management, injury prevention, and Achilles tendon ruptures. With more than six years of clinical experience across neurological, outpatient, and pediatric settings, Dr. Gonzalez combines hands-on expertise with a passion for education. As a writer, he has contributed to fitness publications, newsletters, and rehabilitation courses, with the goal of improving health literacy and breaking down socioeconomic barriers to care.






