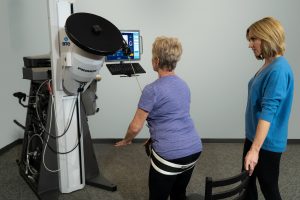
The rehab team at London Road Community Hospital are helping people regain strength and function through Long-COVID so they can get back to work. PrimusRS plays an important role in facilitating functional exercise and providing critical data for patient progress.
The rehab team at London Road Community Hospital are restoring Long-COVID patients’ strength and function for Return to Work using the PrimusRS. They have been using the PrimusRS as part of their highly successful work simulation and functional rehab program, in partnership with local employers. According to Sarah Holt, one of the lead therapists, the ability to customize each evaluation and exercise makes a world of difference for unique work rehab cases like this one.
Continue reading for the full case study and accompanying webinar below, presented by our premiere partners in the UK, Physiquipe.
Return to Work for COVID-19 Patients
Sarah Holt and the Group Rehabilitation Team at London Road Community Hospital in Derby have been using the PrimusRS for over four years. They primarily use the PrimusRS to support musculoskeletal patients in their return to work. They have formed a great income generating partnership with a large local manufacturer using the PrimusRS to provide objective assessment of the employees’ capacity to complete specific work tasks and functional capacity evaluations to support decisions around redeployment.
Since the pandemic has restricted the number of none essential appointments, the team have been using the PrimusRS as part of their objective assessment and remote management of patients. The team have also developed and delivered a rehabilitation pathway for COVID-19 patients aiming to return to work. The impact of the disease can cause substantial long-term issues for the patient. The team’s role is to enable the patient to be able to return to work safely and to reduce the chance of subsequent issues. The PrimusRS is providing vital data to the clinical team, patient and employers to maximise the patients’ recovery and enable them to successfully return to the workplace.
The primary function for Sarah’s team at London Road Community Hospital is to manage the return to work for their patients. The pandemic has meant they have been referred people who have had COVID-19 and are aiming to return to work. The symptoms they have see could manifest itself as an ongoing physical deficit affecting their ability to return to their job or perform specific work tasks.
The rehabilitation team are now able to write ‘fit notes’ which were previously only able to be completed by GPs. These are a lot more comprehensive than GP fit notes as they incorporate specific return o work criteria. This has been a great development for everyone as the team are able to manage this more quickly and devise testing in conjunction with the employers meaning a comprehensive and suitable test.

The common problems COVID-19 patients have presented with are (this is an ever changing list…):
- Weakness
- Breathlessness
- Fatigue – single biggest issue
- Anxiety
- Rapid heart rate
- Joint pain
- Lower rib pain – this appears to be less common
- Headaches is a new complaint
There seems to be more ongoing issues with patients who haven’t had prolonged hospital admissions or been on ICU. Some patients had COVID-19 6 months ago wild ‘mild’ symptoms and are still not able to go back to work. ICU patients are progressing at an expected rate and with the doctors saying recovery pattern seems to be similar to standard pneumonia.. A lot of their patients are female hospital staff in their late 40s and 50s.
It is a big learning curve for them as they normally see MSK patients only.
Case Study
- Female
- 52 year old
- Lives alone
- Diagnosed in April 2020
- Works in hospital as a health care assistant
She was referred by a community physio and started rehab after two months. The main issues were:
- Ongoing breathlessness
- Limited walking tolerance and inability to walk and talk at same time
- High levels of fatigue, anxiety, anger and guilt. Angry with employer at putting her in situation and if this will have an impact on her life, and feeling guilty for not being able to return to work
- Weakness primarily upper limb, reporting difficulties with opening bottles and jars
Initial consultation is via telephone which was an hour and 20 mins which identified ongoing functional issues and task analysis of normal work role and potential difficulties. They initially gave some home exercises relating to functional deficit. They also provided an (electronic) AHP fit note with verbal and written information of fatigue management on COVID-19 specific recovery. They had discussions with respiratory services regarding breathlessness and advised her to self refer to psychological services. She was reluctant to do so but was very glad she did it in the end.
Work Concerns
She had to do a lot of manual handling tasks including pushing wheelchairs, moving equipment, assisting with sit to stand transfers and positioning patients. Communication and social interaction were a key part of the job. Prolonged upper limb activity including operating a scanning machine in a winding motion.
The team decided it would be sensible to have a Covid specific group, this was for the contamination issue but also so they felt supported by the group. This includes cardiovascular exercise, upper limb strengthening work simulated activity, a session with a respiratory physio and techniques to manage this. They would normally have 15 in a group but are now restricted to 6 seeing 24 patients over the course of the day when this would normally be 70.
Outcome Measures – PrimusRS Usage
The PrimusRS plays an important role in being able to dose the patient with the correct resistance and functional tasks. It also provides critical data to be able to progress the patient where necessary. As performance does fluctuate a lot with these patients, it is very important to have the evidence and be able to communicate this with the patient.
Sarah was planning to have a standard evaluation for ever patient but they decided to adapt it to each patients requirements.
The results should that the condition really does fluctuate depending on how the patient is feeling.
They did a rehab session every time she came in on the movements that would help her to be as independent as possible both at home and in work. The tools they used were:
- 162 – grip
- 302 – jar
- 102 – bottle
- 181 – reach
- 181 – rolling patients
- 191 – push/pull
- 701 – short lever position 1- winding the scanner
They also incorporated treadmill and balance training. Sessions lasted 60 minutes with 30 minutes for rehabilitation and 30 minutes for talking.
It is still in the early stages for how rehabilitation will move forward. Sarah’s team will certainly continue with some remote management of their patients on call and video communication. It is still very important to incorporate assessments to ensure that progress is being made.
The COVID-19 pandemic has affected nearly every part of our lives, including the very way may of us work. Rehab professionals around the world are increasingly transitioning to telehealth, altering policies for in-person visits, and finding new ways to optimize their practice during COVID-19. People like Sarah Holt and her team are directly helping patients recover from COVID-19 utilizing innovative technology like the BTE PrimusRS.
As part of our commitment to the therapy community, we have offered multiple treatment guidelines on the safest way to rehab severely deconditioned COVID-19 patients, including sit to stand, active balance and walking, and building strength in lower extremities. Subscribe to TherapySpark to get the latest rehab techniques, resources, and updates, and check out our YouTube channel for more treatment guidelines!
Colleen Isaiah
TherapySpark Editor
BTE