The Ultimate Guide to the Craniocervical Flexion Test (CCFT): Drive Objective Outcomes and Differentiate Your Practice
Treatment GuidelinesMaster the Craniocervical Flexion Test with a step-by-step protocol to assess deep cervical flexor function, generate objective neck strength data, and build measurable, data-driven treatment plans for patients with neck pain.
The Craniocervical Flexion Test (CCFT) assesses deep cervical flexor muscle control, providing objective data for neck pain evaluations and treatment planning. This guide covers a complete CCFT protocol, interpretation methods, and how to build data-driven neck pain treatment plans. Learn how to standardize assessment across your practice, improve documentation for reimbursement, and leverage technology for enhanced outcomes and efficiency.
The CCFT transforms subjective neck pain assessment into quantifiable, trackable outcomes that benefit both patients and your practice.
Moving Beyond Subjectivity in Neck Pain Assessment
If you’re like most clinicians, you’ve faced the challenge of quantifying neck pain improvement. Your patient tells you they feel “better,” but how do you document that progress objectively? How do you prove to insurers that your treatment works? The Craniocervical Flexion Test changes this narrative entirely.
The CCFT provides the objective, reproducible data you need to evaluate deep cervical flexor function, track patient progress, and justify your treatment approach. This guide goes beyond basic test administration: we’ll show you how to leverage the CCFT to improve clinical outcomes, streamline your workflows, and strengthen your practice’s position in an increasingly competitive market.
Whether you’re a practitioner seeking clearer protocols, a clinic owner focused on differentiation, or an administrator working to standardize care across multiple sites, this comprehensive guide delivers the practical insights you need.
Why the CCFT is a Non-Negotiable Tool for Modern Rehab
The deep cervical flexors, specifically the Longus Colli and Longus Capitis muscles, serve as the foundation of cervical spine stability. These muscles provide segmental control and maintain optimal cervical posture during daily activities. When these muscles fail to activate properly, patients compensate with superficial muscles like the sternocleidomastoid and scalenes, creating inefficient movement patterns that perpetuate pain and dysfunction.
Research consistently links deep cervical flexor dysfunction to chronic neck pain, cervicogenic headaches, and whiplash-associated disorders. The CCFT allows you to objectively measure this dysfunction, providing quantifiable baseline data that guides your entire treatment approach.
Clinic Differentiation and Reimbursement
For clinic owners and managers, the CCFT offers more than clinical value: it strengthens your operations. Objective assessment data provides quantifiable proof of impairment and progress, supporting cleaner reimbursement claims. When you document a patient’s progression from 22 mmHg to 28 mmHg activation over four weeks, you’re providing insurers with concrete evidence that justifies continued care.
This objective approach also differentiates your practice. While competitors rely on subjective pain scales, you’re delivering measurable, reproducible outcomes that resonate with referring physicians, employers, and payers.
Mastering the CCFT: A Step-by-Step Protocol for Reliable Results
Equipment and Patient Setup
Position your patient supine with knees bent and feet flat on a treatment table. Place a folded towel under the occiput to maintain neutral cervical spine alignment. A pressure biofeedback unit (PBU) goes behind the neck, positioned at the cervical lordosis. Inflate the PBU to 20 mmHg as your baseline.
The Standardized Two-Stage Protocol
Stage 1: Activation Assessment
Guide your patient through a gentle nodding motion, as if saying “yes” slowly. The goal is progressive pressure increases without engaging superficial muscles. Target these levels sequentially:
- 22 mmHg: Hold for 2-3 seconds
- 24 mmHg: Hold for 2-3 seconds
- 26 mmHg: Hold for 2-3 seconds
- 28 mmHg: Hold for 2-3 seconds
- 30 mmHg: Hold for 2-3 seconds
Stage 2: Endurance Testing
Once you identify the highest pressure level achieved without compensation, test endurance. Have your patient perform 10-second isometric holds at this level. Count the number of successful repetitions completed before fatigue or compensation occurs.
Critical Detail: Identifying Compensatory Strategies
Watch for these common compensation patterns that indicate superficial muscle overactivity:
- Visible contraction of the sternocleidomastoid
- Excessive chin retraction
- Loss of neutral spine position
- Breath holding
- Scalene muscle activation (palpate laterally)
When you observe compensation, that’s your ceiling for that patient’s current capacity. Document this level as their baseline score.
Interpreting the Data: From Numbers to Actionable Clinical Insights
Scoring the Test
Your CCFT assessment yields two critical metrics:
Activation Score: The highest pressure level (22-30 mmHg) the patient achieves with proper form. A score of 26 mmHg or below typically indicates significant deep cervical flexor dysfunction requiring targeted intervention.
Performance Index: The number of successful 10-second holds completed at the maximum pressure level. For example, “3/10 repetitions at 26 mmHg” provides both activation and endurance data.
Telling a Clear Story with Data
These objective scores become powerful communication tools. For practitioners, the data pinpoints the exact nature of motor control deficits, distinguishing between activation problems versus endurance limitations.
For all stakeholders, these numbers create a clear narrative. You can show a workers’ compensation carrier that an injured employee progressed from 22 mmHg activation to 28 mmHg over six weeks, directly correlating with functional improvements. This objective progression supports continued care authorization and demonstrates treatment effectiveness.
From Assessment to Action: Building a Data-Driven Treatment Plan
Progressive Exercise Prescription Based on CCFT Score
Your CCFT results directly inform your treatment progression:
Low Score (22-24 mmHg):
Start with basic craniocervical flexion activation exercises without pressure targets. Focus on motor control retraining using tactile and verbal cues. Progress to gravity-eliminated positions if needed. Consider incorporating BTE’s Multi-Cervical Unit for controlled, progressive strengthening with objective force measurements.
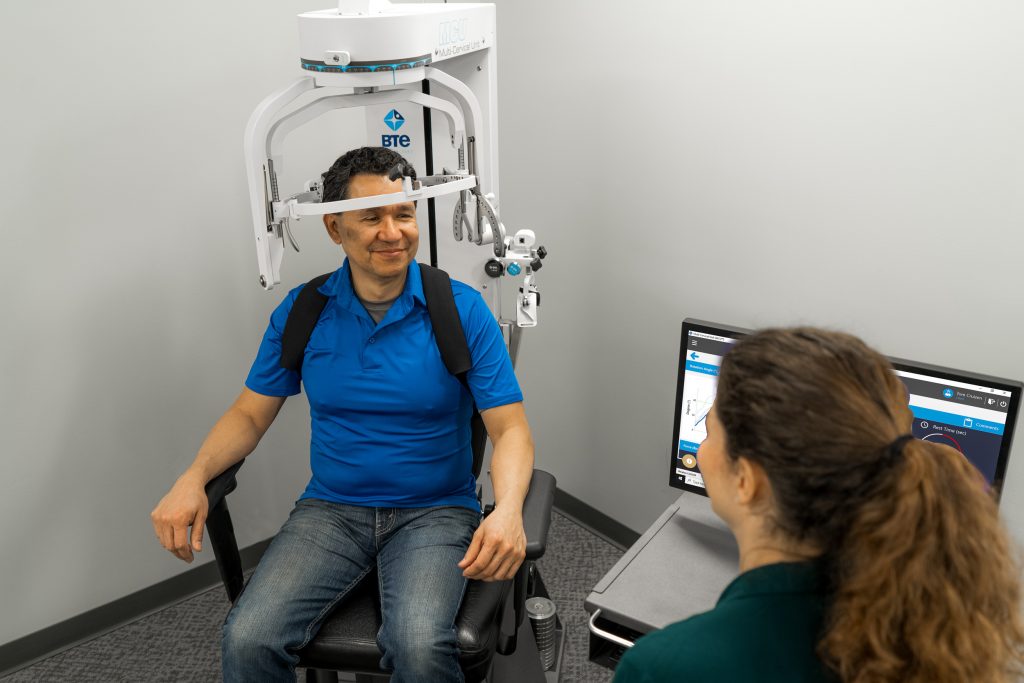
Moderate Score (26-28 mmHg):
Introduce targeted pressure holds using the PBU for feedback. Begin endurance training with multiple repetitions at submaximal levels. Add gentle isometric resistance in multiple planes to challenge stability while maintaining deep flexor activation.
High Score (30 mmHg):
Progress to functional integration exercises. Combine deep cervical flexor activation with upper extremity movements to simulate work or sport demands. The MCU system helps clinicians provide precise resistance training across all cervical motions while providing objective measurement of strength gains.
Application for Specialized Populations
For Occupational Health and Workers’ Compensation:
Link CCFT scores directly to functional capacity. A warehouse worker requiring sustained cervical positioning needs different endurance benchmarks than an office worker. Use progressive CCFT improvements to justify return-to-work timelines with objective data.
For Sports Medicine:
Athletes in contact sports or those performing overhead activities require superior cervical motor control. Establish sport-specific CCFT benchmarks: a gymnast might need consistent 30 mmHg activation with 10/10 endurance before return-to-sport clearance.
Beyond the PBU: Modernizing the CCFT for Efficiency and Precision
The Limits of Analog Assessment
Traditional pressure biofeedback units serve their purpose, but they present challenges. Inter-rater reliability varies when different clinicians read analog gauges. Manual documentation takes time and introduces transcription errors. Tracking progress across sessions requires meticulous record-keeping that many busy clinics struggle to maintain.
The Digital Advantage
Modern cervical assessment technology transforms the CCFT from a simple test into a comprehensive evaluation system. Digital pressure sensors provide precise, repeatable measurements that eliminate subjective interpretation. Real-time visual displays engage patients by showing their performance instantly, improving motor learning and compliance.
For practitioners, automated data capture means spending less time documenting and more time treating. The Multi-Cervical Unit exemplifies this approach, allowing clinicians to assess cervical strength and ROM objectively across all planes of motion while automatically generating progress reports.
Clinic owners and managers benefit from technology’s ROI through improved throughput and premium service offerings. When you can show patients their objective progress on a screen, justify your fees with comprehensive reports, and demonstrate superior outcomes to referral sources, you strengthen your market position.

Integration with Comprehensive Evaluation
Consider how the CCFT fits within your broader assessment strategy. Pairing deep cervical flexor testing with comprehensive strength and range of motion evaluation provides the complete picture needed for evidence-based treatment planning. Systems like BTE’s functional rehabilitation line help clinicians capture objective data across multiple domains, creating robust documentation that satisfies the most stringent requirements.
Standardize, Quantify, and Excel
The Craniocervical Flexion Test represents more than an assessment tool: it’s your gateway to objective, data-driven cervical spine rehabilitation. By mastering the CCFT protocol, you transform subjective complaints into measurable impairments that guide targeted treatment.
We’ve shown you how proper CCFT implementation improves clinical decision-making, strengthens documentation, and differentiates your practice. The combination of standardized protocols and modern technology positions you to deliver superior outcomes while operating more efficiently.
Your patients deserve treatment based on objective data, not guesswork. Your practice deserves the competitive advantage that comes from proving your value with concrete results. The CCFT, especially when enhanced with modern assessment technology, provides both.Ready to elevate your cervical assessment beyond basic manual testing? Discover how BTE’s Multi-Cervical Unit helps clinicians standardize cervical evaluation, automate documentation, and deliver the objective insights that drive superior outcomes. Contact us today to learn how objective assessment technology can transform your approach to cervical rehabilitation.
Craniocervical Flexion Test FAQs
What equipment do I need to perform the Craniocervical Flexion Test?
You need a pressure biofeedback unit (PBU), also called a stabilizer or pressure cuff, which can be inflated and displays pressure readings in mmHg. The patient should be positioned on a treatment table that allows for comfortable supine positioning. Some clinics also use a towel roll under the neck for additional support, though this isn’t always necessary. Ensure the PBU is properly calibrated and functioning before each use.
How do I know if a patient is compensating during the test?
Watch for these common compensation patterns: visible activation of the sternocleidomastoid or anterior scalene muscles (you’ll see muscle bulging or neck straining), lifting of the head off the table, jaw clenching or teeth grinding, breath holding, or loss of the neutral cervical curve. The movement should be a gentle nodding motion isolated to the upper cervical spine, not a general neck flexion. If you observe any of these compensations, the patient has reached their maximum non-compensated level.
What’s considered a normal vs. abnormal result on the CCFT?
Healthy individuals typically can reach and hold 26-30 mmHg without compensation for the full 10 seconds. Patients with neck dysfunction often struggle to reach or maintain pressures above 22-24 mmHg without compensating. However, focus more on the quality of movement and absence of compensation rather than just the pressure number. A patient who can only reach 22 mmHg cleanly may have better deep cervical flexor function than someone who reaches 28 mmHg with significant compensation.
Can I use the CCFT as both an assessment and treatment tool?
Yes, the CCFT serves dual purposes. As an assessment, it helps identify deep cervical flexor dysfunction and establishes baseline measurements for progress tracking. As a treatment intervention you can use the same setup for therapeutic exercises, having patients practice controlled activation at their appropriate pressure level. Start with 5-second holds and gradually progress duration and pressure as their control improves. This makes it an efficient and cost-effective tool for your clinic.
Are there any contraindications or precautions for performing the CCFT?
Avoid the CCFT in patients with acute cervical spine injuries, suspected fractures, severe cervical instability, or acute torticollis. Use caution with patients who have severe headaches, dizziness, or vertigo, as the test position may exacerbate symptoms. Pregnant patients in later trimesters may find the supine position uncomfortable. Always ensure patients can tolerate lying flat and can communicate any discomfort during the test. Stop immediately if patients report increased pain, dizziness, or neurological symptoms.
How should I document and track CCFT results for insurance and progress notes?
Document the maximum pressure achieved without compensation (e.g., “24 mmHg”), the hold time if less than 10 seconds (e.g., “held for 6 seconds”), and note any compensation patterns observed. Include functional correlations like “patient reports decreased neck stiffness with improved CCFT performance from 20 to 26 mmHg over 4 visits.” For insurance purposes, tie results to functional outcomes and treatment goals. Track changes over time to demonstrate objective progress, which supports continued treatment authorization and validates your intervention effectiveness.