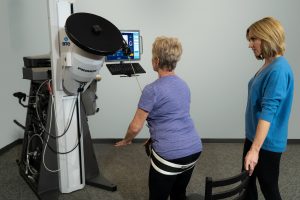
Preventive exercise programs may be able to reverse the trend. But only if they effectively address the root causes. Here you’ll find a review of the literature on fall risks for older adults and interventions that can help prevent fall-related deaths.
You Can Help Reverse the Trend
Fall incident data from the CDC shows an alarming trend – older adults are dying from fall-related injuries at increasing rates. The fall-related death rate rose by 30% between 2009 and 20181. Fall risks are a concern for just about everyone working in rehabilitation. Even if it doesn’t lead to death, a fall can often mark the beginning of a difficult period of severe injury, loss of function, extended hospital stays, and major lifestyle changes.
Preventive exercise programs may be able to reverse the trend2. But only if they effectively address the root causes. Here you’ll find a review of the literature on fall risks for older adults and interventions that can help prevent fall-related deaths.
Statistics on Fall-related Injuries
Falls are one of the most widespread injury concerns for the elderly. More than one in four people over the age of 65 fall each year, according to the CDC3. On top of that, one in five falls causes a serious injury, such as a bone fracture or head injury. Looking at hip fractures alone, falls account for more than 95% of them. They’re also one of the leading causes of traumatic brain injury3.
Falls are associated with increased utilization of healthcare resources, longer lengths of stay, and poorer health conditions overall. Minor fractures and soft tissue injuries can cause significant dysfunction, pain and distress. Any falls – even minor falls – can trigger feelings of fear that leads older adults to limit their physical activity, which leads to loss of strength and independence3.
Fall Risk Factors
The CDC lists several fall risk factors, such as lower extremity weakness and difficulty with walking and balance. Older adults who have fallen in the past have a high risk of falling again. A history of falling is the first item listed on the Morse Fall Scale4, a form that helps medical professionals assess a patient’s risk of falling.
Fall-related Deaths Increasing for Older Adults
Healthcare professionals have been working to reduce the number of falls among older adults. Despite their best efforts, the number of fall-related deaths among seniors is rising1,5. The risk increases further as people age. One study shows that the mortality rate for people aged 75-79 is 42 out of 100,000. The rate increases to 590 for people aged 95 and older5.
It is possible that today’s older adults are more vulnerable to falls because they are living longer. Older adults are also more likely to have chronic health conditions associated with an increased risk of falls, such as diabetes6 and cardiovascular disease7.
Improving Balance and Lower Extremity Strength
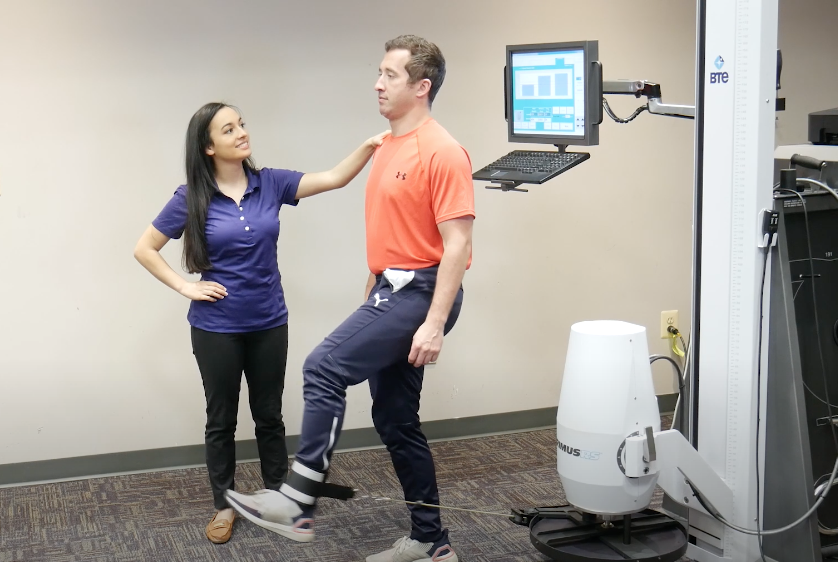
The best way to prevent falls is to address the underlying biomechanical cause. For most people, the issue is a lack of balance and lower extremity strength. We recently posted a video that shows you how to strengthen all the major joints involved in walking – ankles, knees, and hips – with eccentric exercise on the PrimusRS. You’ll also learn how the Primus can help you improve active balance with an assisted walking exercise. These exercises are safe enough for frail or elderly clients to gradually build stability and confidence. Watch the video to learn more.
Fall Prevention with the Otago Method
Another article published in JAMA supports the use of Physical Therapy programs to prevent falls. This study looked at the effectiveness of the Otago exercise program, a fairly new development in senior care.
Developed in New Zealand, Otago is a series of 17 strength and balance exercises that aims to reduce falls in frail older adults. According to the Carolina Geriatric Education Center, it can reduce the risk of falls by as much a 30-40%8. The National Council on Aging9 (NCOA) considers Otago “one of the most appropriate fall prevention programs for older adults who are frail and may not be able to participate in a group-based program like Tai Chi.”
To study this method, the team randomly assigned 345 participants who had recently seen a physician for a fall into either the exercise group or a control group. The participants in the control group received 12 months of traditional treatment. This included medical and fall risk assessments, treatment and lifestyle recommendations by a geriatrician, and referrals to other healthcare providers as needed.
The participants in the Otago group received usual care plus the home-based Otago exercise program. This group completed the exercises three times aper week and walked for 30 minutes every week. The researchers returned to the participants’ home every other week to adjust the exercises. All participants underwent physician evaluations at 6 and 12 months8.
Reducing the Risk of Fall-related Death
The authors of the study found a significant reduction in falls among participants who completed the Otago program. The rate for the Otago group was 1.4 per person/year, and the traditional care group had a rate of 2.1. There were no significant differences between the two groups when it came to general balance and mobility8.
The authors note that, while older adults clearly have the highest risk for falls, people in this age group “also have the highest potential for cost-effective interventions that make a difference8.” Physical therapy, occupational therapy, and other types of rehabilitation can improve patient safety and patient outcomes.
Fall Prevention With Eccentric Exercise
Eccentric exercise is one of the best modalities for frail or elderly clients. It puts less strain on the body than concentric exercise, so they can tolerate it better. Traditional exercises usually include both an eccentric and concentric phase of contraction, but there is a way to achieve ONLY eccentric contractions: with the Eccentron.
Think of it as the opposite of a leg press. Instead of pushing pedals concentrically, the client resists as the pedals move toward them. They’re doing all the resistance as knees move to chest and relaxing as the leg extends. Exercising under an eccentric load allows the muscle to lengthen under force and gradually build lower extremity strength.
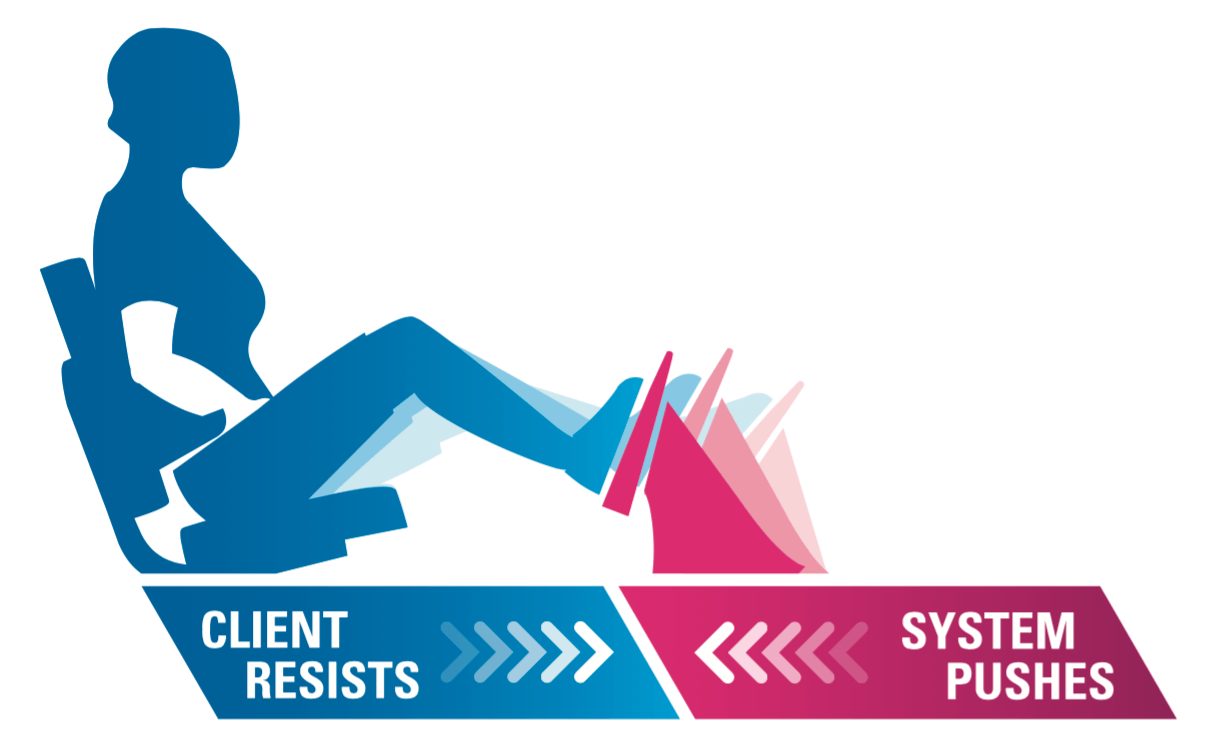
With the Eccentron, you can load as little as a fraction of the client’s bodyweight. That makes it safe even for your most frail clients. Learn more about strengthening the lower extremities with the Eccentron here.
More Fall Prevention Resources
If you work with an at-risk population, check out our additional resources on preventing fall-related death and injury:
- Video: Walking and Active Balance Exercises for Severely Deconditioned Patients
- Video: Lower Extremity Strengthening for Cardiorespiratory / Deconditioned Patients
- Sarcopenia Prevention with Eccentric Exercise
References
- Centers for Disease Control and Prevention, National Center for Injury Prevention and Control. Web-based Injury Statistics Query and Reporting System (WISQARS) [online].
- Liu-Ambrose, T. 2019 Effect of a Home-Based Exercise Program on Subsequent Falls Among Community-Dwelling High-Risk Older Adults After a Fall: A Randomized Clinical Trial. JAMA Network. https://jamanetwork.com/journals/jama/article-abstract/2735075
- Important Facts about Falls. 2017. Centers for Disease Control and Prevention (CDC).
- Morse Fall Scale. 2013. Agency for Healthcare Research and Quality. https://www.ahrq.gov/professionals/systems/hospital/fallpxtoolkit/fallpxtk-tool3h.html
- Hartholt, K.A. 2019. Mortality From Falls Among US Adults Aged 75 Years or Older, 2000-2016. JAMA Network. https://jamanetwork.com/journals/jama/article-abstract/2735063#
- Yang, Y. 2016. Diabetes mellitus and risk of falls in older adults: a systematic review and meta-analysis. Age and Aging. https://www.ncbi.nlm.nih.gov/pubmed/27515679
- Manemann, S.M. 2018. Fall Risk and Outcomes Among Patients Hospitalized With Cardiovascular Disease in the Community. Circulation. https://www.ahajournals.org/doi/10.1161/CIRCOUTCOMES.117.004199
- The Otago Exercise Program. 2019. Carolina Geriatric Education Center (CGEC). https://www.med.unc.edu/aging/cgec/exercise-program/
- Otago Exercise Program Guidance Statement. 2017. National Council on Aging (NCOA).