
Building a Data-Driven, High-Performance Stroke Rehabilitation Exercise Program
Treatment GuidelinesExplore stroke rehab exercises and data-driven protocols that boost patient outcomes, streamline clinic workflow, and support reimbursement.
Stroke rehabilitation requires more than just a list of exercises. Building a successful program means combining evidence-based protocols with objective data collection and strategic technology use. This comprehensive approach helps clinics differentiate their services, demonstrate clear value to payers, and achieve consistent patient outcomes. By focusing on early intervention, standardized yet flexible protocols, and measurable progress tracking, your clinic can transform stroke rehabilitation from a standard service into a center of excellence that drives both clinical success and business growth.
From Stroke Recovery to Exceptional Care
If you’re running a physical or occupational therapy clinic, you know that stroke rehabilitation exercises form the backbone of recovery for millions of patients each year. While most clinics offer some form of stroke rehab, many struggle to differentiate their services, demonstrate clear value to payers, and achieve consistent, optimal outcomes.
Here’s the opportunity: stroke rehabilitation represents significant potential for business growth. A strategic, evidence-based program positions your clinic as a market leader, not just another provider offering basic services.
This guide moves beyond simple exercise lists to provide a comprehensive framework for building a superior stroke rehabilitation program. We’ll explore how to leverage evidence, technology, and objective data to drive better clinical outcomes, improve operational efficiency, and secure financial success.
Why Early, Targeted Stroke Rehab Benefits Patients and Your Clinic
Harnessing Neuroplasticity: The ROI of Early and Intensive Intervention
The concept of the “golden window” of neuroplasticity isn’t just clinical theory; it’s a program driver. During the first few months after stroke, the brain shows remarkable capacity for reorganization. Brain-derived neurotrophic factor (BDNF) levels increase with exercise, promoting neural recovery and cognitive function restoration.
When you structure your program around this principle, you achieve faster recovery and superior outcomes. This creates a powerful marketing message that attracts referrals and differentiates your clinic. Hospital systems and referring physicians want to send patients to clinics that understand and capitalize on this critical recovery period.
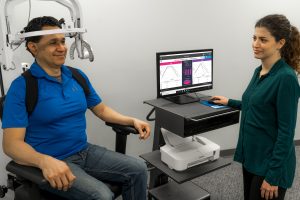
Your clinicians can leverage tools like one of our most popular systems, the PrimusRS to provide task-specific training during this crucial window. The system helps clinicians deliver multi-joint functional rehabilitation with objective assessments, ensuring that every session maximizes neuroplastic potential while capturing measurable progress data.

The Cost of Inaction and Generic Programming
When stroke rehabilitation exercises aren’t implemented effectively, patients experience prolonged recovery times, increased secondary complications, and poor satisfaction scores. These outcomes lead to longer care episodes, potential insurance denials, and weakening of your clinic’s reputation.
Consider the cascade effect: inadequate early intervention leads to compensatory movement patterns, which become harder to correct over time. This extends treatment duration, frustrates patients, and complicates reimbursement justification. By implementing a comprehensive, data-driven approach from day one, you prevent these costly complications.
Personalization as a Protocol
Every stroke patient presents unique challenges, yet your clinic needs standardized processes for efficiency. The solution lies in creating flexible protocols that ensure personalized care within a systematic framework.
This means establishing clear assessment protocols, defining progression criteria based on objective measurements, and creating decision trees that guide treatment modifications. Your team benefits from consistent workflows while patients receive individualized care plans that address their specific deficits and goals.
An Successful Exercise Framework
Building Blocks: Foundational Movement and Strength Training
Every successful stroke rehabilitation program starts with the fundamentals. Range of motion exercises, flexibility training through controlled stretching, and basic strengthening form the non-negotiable foundation. These exercises prevent contractures, maintain joint health, and prepare tissues for more complex movements.
Your clinicians should begin with passive range of motion, progressing to active-assisted and then active movements as motor control returns. Resistance training starts with gravity-eliminated positions, advancing to anti-gravity work using bands, weights, and bodyweight exercises.
Our Multi-Cervical Unit (MCU) helps clinicians address often-overlooked cervical deficits in stroke patients. The system provides objective evaluation and strengthening with controlled positioning, essential for patients with neglect or postural control issues affecting head and neck alignment.
Rebuilding Motor Control: Integrating Advanced Methodologies
Moving beyond basic exercises requires understanding and applying evidence-based motor learning approaches. Here’s how to integrate these methodologies into your stroke rehabilitation exercises:
Neurodevelopmental Treatment (NDT/Bobath Approach): This method helps normalize muscle tone and facilitate functional movement patterns. Your therapists use handling techniques to guide patients through normal movement sequences, inhibiting abnormal patterns while encouraging proper motor control. This approach works particularly well when combined with objective strength measurements that track progress in specific muscle groups.
Constraint-Induced Movement Therapy (CIMT): For patients with learned non-use of the affected limb, CIMT provides an intensive protocol. By constraining the unaffected limb and focusing repetitive practice on the affected side, clinicians help patients overcome compensatory strategies. Our Capri device enhances this approach by providing gamified hand therapy that maintains patient engagement during these intensive sessions, helping clinicians deliver neuromuscular control and motor retraining.

Stage-Specific Motor Recovery: Understanding the stages of motor recovery guides exercise prescription. From initial flaccidity through synergistic movements to isolated control, each stage requires specific interventions. Your protocols should define clear criteria for progression between stages based on objective measurements.
Mastering Function: From Clinic Drills to Real-World Independence
Functional training bridges the gap between isolated exercises and real-world activities. Task-specific practice remains the gold standard for motor learning, with repetition and context driving neuroplastic changes.
Key functional exercises include:
- Sit-to-stand training for fundamental mobility
- Transfer practice for bed, chair, and car mobility
- Gait training with progressive challenges
- Upper extremity tasks mimicking daily activities
The Simulator II helps clinicians replicate job tasks and activities of daily living with objective documentation. This system allows your team to progress patients from basic movements to complex, coordinated activities that directly translate to independence at home and work.
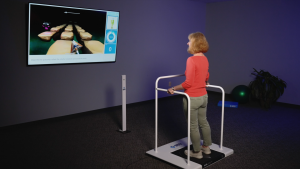
Balance training deserves special attention in stroke rehabilitation. The Alfa balance platform helps clinicians test and address balance dysfunction with therapeutic gaming. It leverages key aspects of stroke rehabilitation: task-oriented movement, high repetition, and visual engagement that drives neuroplastic changes.
Leveraging Data and Technology to Elevate Stroke Rehabilitation Exercises
Objective by Design: Measuring What Matters for Reimbursement and Results
Here’s where your program separates from the competition. While other clinics rely on subjective observations and manual muscle testing, you implement objective measurement at every stage. This approach provides clinicians with clear progress markers, gives owners the documentation needed for cleaner reimbursement, and supplies administrators with compliance and performance data.
Start by establishing baseline measurements for:
- Isometric and dynamic strength across affected muscle groups
- Active and passive range of motion
- Balance and postural control metrics
- Functional task performance times and quality
Using Technology to Boost Stroke Rehab Results
Technology doesn’t replace skilled clinicians; it amplifies their effectiveness. Modern rehabilitation technology serves three critical functions in stroke recovery:
Patient Engagement: Gamification and real-time feedback maintain motivation during repetitive exercises. Visual displays showing performance metrics help patients understand their progress, increasing adherence to prescribed protocols.
Extended Therapy: Home exercise programs with objective tracking extend therapy beyond clinic walls. Patients continue therapeutic activities between sessions, maximizing recovery during the critical neuroplastic window.
Increased Throughput: Technology enables therapists to manage larger caseloads effectively. While one patient works independently on technology-assisted exercises with built-in safety features, the therapist provides hands-on treatment to another patient.
The Eccentron exemplifies this approach for lower extremity training. The system helps clinicians provide eccentric resistance training, which uses less oxygen and reduces fatigue while allowing higher loading capacity. This enables intensive strength training even for patients with cardiovascular limitations common after stroke.
Quantifying Readiness: Data for Return-to-Work and Return-to-Life
Objective data transforms vague recovery goals into concrete milestones. Instead of telling families their loved one is “getting stronger,” you show specific strength gains, improved reaction times, and functional capacity improvements.
For occupational health directors and workers’ compensation coordinators, objective metrics provide clear return-to-work criteria. The Evaluator portable testing kit enables on-site functional assessments, bridging the gap between clinic-based rehabilitation and workplace demands.
Consider implementing standardized testing protocols at regular intervals:
- Initial evaluation within 72 hours of admission
- Weekly progress assessments during acute phase
- Bi-weekly measurements during subacute recovery
- Monthly evaluations during chronic management
These objective measurements support clinical decisions about exercise progression, justify continued therapy to payers, and provide patients with tangible evidence of improvement.
Building Your Program Implementation Strategy
Successfully implementing a data-driven stroke rehabilitation program requires systematic planning. Start by auditing your current capabilities and identifying gaps in equipment, training, or protocols. Develop standardized assessment and treatment protocols that incorporate objective measurement at defined intervals.
Train your team not just on exercise techniques, but on the business value of objective documentation. Help them understand how data supports both clinical excellence and financial sustainability. Create workflows that integrate technology seamlessly without disrupting patient care.
Market your enhanced capabilities to referral sources. Hospitals and physicians value clinics that provide detailed, objective progress reports. Insurance companies appreciate clear documentation supporting medical necessity. Patients and families gain confidence from seeing measurable improvement.
Conclusion: Build Your Stroke Exercise Program for Clinical and Business Success
A leading stroke rehabilitation program rests on three pillars: evidence-based exercise protocols, objective data capture at every stage, and strategic technology integration. This systematic approach helps clinic owners grow revenue through improved outcomes and cleaner reimbursement. Clinicians achieve better results with clear, measurable goals. Administrators standardize excellence across their facilities.
Your stroke rehabilitation exercises become more than just movements; they become part of a comprehensive system designed for success. By combining traditional therapeutic approaches with modern objective assessment tools, you create a program that stands out in the marketplace while delivering superior patient outcomes.
Ready to transform your stroke rehabilitation services into a data-driven center of excellence? Discover how BTE’s comprehensive rehabilitation and evaluation systems provide the objective assessment tools, evidence-based protocols, and patient engagement features you need to lead the way in stroke recovery. Your patients deserve the best possible outcomes, and your clinic deserves the tools to deliver them.
Stroke Rehabilitation Exercises FAQ
Q: How soon after a stroke should rehabilitation exercises begin, and what factors determine the starting point?
A: Rehabilitation should ideally begin within 24-48 hours post-stroke, once the patient is medically stable. The timing depends on stroke severity, consciousness level, blood pressure stability, and absence of active bleeding. Early mobilization, even passive range of motion exercises in bed, helps prevent complications like blood clots, pneumonia, and muscle contractures. However, patients with severe deficits may need to start with basic positioning and progress gradually. Always coordinate with the medical team and follow physician clearance protocols before initiating any exercise program.
Q: What’s the difference between spasticity and flaccidity in stroke patients, and how do exercise approaches differ for each?
A: Flaccidity occurs immediately post-stroke when muscles are completely limp with no tone, typically lasting days to weeks. During this phase, focus on passive range of motion, proper positioning, and gentle facilitation techniques to prevent contractures. Spasticity develops later as tone returns but becomes excessive and uncontrolled. For spastic muscles, use sustained stretching, weight-bearing activities, and inhibition techniques from the Bobath approach. Avoid quick stretches or aggressive movements that can trigger spastic responses. The Brunnstrom stages help track this progression from flaccidity through spasticity to voluntary control.
Q: How do you determine if a stroke patient is appropriate for Constraint-Induced Movement Therapy (CIMT)?
A: CIMT candidates must have at least 20 degrees of active wrist extension and 10 degrees of finger extension in the affected hand. They need adequate cognitive function to follow multi-step instructions and participate in 2-6 hours of daily practice. Patients should be at least 3 months post-stroke with plateau in traditional therapy. Exclude patients with severe cognitive impairment, uncontrolled medical conditions, severe depression, or significant pain. Modified CIMT with shorter practice periods may be appropriate for patients who don’t meet full criteria but show some voluntary movement in the affected limb.
Q: What are the key safety considerations when implementing balance training for stroke patients?
A: Always use appropriate fall prevention measures including gait belts, spotting techniques, and nearby grab bars or parallel bars. Start with seated balance activities before progressing to standing. Ensure patients wear proper footwear with good traction and remove trip hazards from the treatment area. Monitor for orthostatic hypotension, especially during position changes. Be aware of visual field deficits, neglect, or perceptual issues that increase fall risk. Progress exercises gradually from stable to unstable surfaces, and always have emergency protocols in place. Document baseline balance assessments using standardized tools like the Berg Balance Scale.
Q: How do you modify exercises for stroke patients with cognitive impairments or aphasia?
A: Break complex tasks into simple, single-step instructions and use demonstration rather than lengthy verbal explanations. Provide visual cues, pictures, or physical guidance to supplement verbal instructions. Allow extra processing time and repeat instructions as needed. For patients with aphasia, use yes/no questions, gestures, and written cues when appropriate. Establish consistent routines and use the same terminology across therapy sessions. Consider cognitive load – if working on motor skills, minimize cognitive demands, and vice versa. Involve family members to reinforce instructions and provide familiar communication patterns.
Q: What documentation and outcome measures are essential for tracking progress in stroke rehabilitation?
A: Use standardized assessments like the Fugl-Meyer Assessment for motor function, Berg Balance Scale for balance, and Functional Independence Measure (FIM) for daily activities. Document baseline measurements within the first few sessions and reassess at regular intervals (typically every 2-4 weeks). Track specific, measurable goals such as “patient will independently transfer from bed to wheelchair” rather than vague statements. Include safety considerations, equipment needs, and level of assistance required. Document any adverse events, patient tolerance, and modifications made to exercises. Insurance often requires functional outcome measures to justify continued treatment, so maintain detailed progress notes linking exercises to functional improvements.




